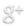How the consultation room may drive your Patient retention
In this the third article I would like to move on to the consultation room, initially I would like the cover the environs of the room but also the consultation practice itself. I shall attempt to cover the room and the structure of the consultation in this article and explore the consultation in a deeper manner in the next. We have reached the consultation room, the inner sanctum, the place where we have traditionally thought the real action occurs. It is indeed all of those things, but I hope I have showed in my previous articles that it is indeed not the whole story when it comes to Patient journey and engagement.
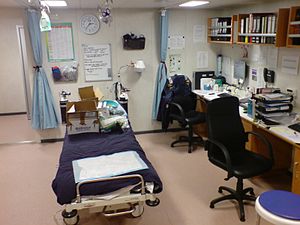
When you enter your consultation room, take a good look around it and ask yourself, what does this room say about me and my day to day practice? I undertook this exercise after I had been in practice for a while, initially when I started my practice day to day thoughts just centred on my audiometery and hearing instrument fitting, my main worry was that I did not make a mess of these elements. After I had settled down and realised I was the king of practice, sorry can’t resist. I began to concentrate on the sales elements that we all undertake in our consultations, slowly but surely finding my consultation style. With this done I began to look at my consultation room, it’s appearance and design and how I could change that to engender the perception I wished and allow me to connect with my Patients.
I realised that my consultation room was a mess, between hanging cables, the bane of our existence these, tackle boxes full of tubing etc the usual day to day detritus of a practice. I also realised that I sat behind a desk, talking to my Patients, when I thought about this clearly it seemed immediately the wrong position to be in if I was trying to engage with my Patients. So with this in mind, take a long look at your consultation room, store your cables and paraphernalia out of site, whatever you use during one consultation, put it away afterwards. The only things that should be visible on your desk are the fixed apparatus that we use every day. An audiometer, a computer monitor and a keypad, your otoscope and very little else.
If you do not have proper storage, get some built in or indeed buy a nice piece of furniture to store everything in, keep it tidy and keep everything in its place. There is nothing worse than searching like an idiot for something whilst your Patient looks on. Change your desk aspect; place it in order that the Patient and their significant other sit beside you as opposed to across from you. This allows a greater feeling of engagement with your Patient, it also closes the physical gap between you and them, allowing the Patient to relax somewhat and as the consultation moves on to emotionally engage with you in an easier manner.
Position the equipment on your desk including your computer screen and keyboard in an aspect that always allows you to be looking towards the Patient and the significant other. This allows constant engagement with both of them, if you want real long term commitment from your Patient you will need to engage with their companion/family also. This is imperative; engagement with the Patient’s companion will increase the commitment to you and your advice from the Patient. That engagement needs to start from the initial consultation, if not during the actual making of the appointment.
The Walls of your consultation room also need to be looked at strongly, do you have anatomical display posters, and are they properly farmed and hung? Again do you have manufacturer posters, are they properly framed and do you update them? If you do indeed have manufacturer posters, why do you? I am still unsure if it is indeed a good idea to have such marketing elements in a consultation room, having those elements does not speak of an independent clinician. Having half a dozen of the different Manufacturer posters speaks of a supermarket, I am not sure if there is an in-between so hang a nice relaxing picture instead and of course your qualification.
Keep it clean and tidy, tidy up during the day if need be, you wish to be perceived as a consummate professional with a deep sense of empathy and caring, you need to display that consistently. Before you open your mouth, your practice initial communications and the deportment of your staff has already said a great deal.
In order to have a maximum effect, the actual consultation needs to be well planned and enacted, in the planning stage you need to think strongly about Patient perception and psychology and what indeed you hope to achieve. Whilst Audiologists or Dispensers are mostly caring and motivated by the opportunity to make a real difference to somebody’s life, we got to eat, so assisting somebody is balanced with making a sale. Most of our Patients, do not want to buy, in fact the last thing they generally want is hearing aids. It is with this fact in mind that we see the challenge we face every day, how do you convince somebody that they need a product they do not want without falling back on the optimal negotiation position (the head lock for those who don’t know).
With these stark facts in mind you need to design a consultation that allows you to convince them of the benefits of a device without any perception of a hard sell. This is possible, not only is it possible but there are gifted Dispensers doing it with effortless ease every day on instinct, for you and me I am afraid we have to work at it. You may think that planning a consultation to influence people surreptitiously is underhanded, but if like me, you think you are an excellent clinician who deeply cares for your Patient. Does it not follow that you should undertake every possible action and explore every avenue to ensure a Patient comes into and stays in your care?
The stages of a consultation are qualifying to see in fact if a Patient has a loss, overcoming objections to meet any queries, worries or objections that a Patient or indeed the significant other has and closing the sale. The consultation does not necessarily fall in that order, the initial part of the consultation should be a mixture of qualifying and overcoming objections which leads to testing and then the close. Think deeply about this process, come to conclusions and then design a medical record card that follows the flow that you have chosen and includes headlines that cover all the questions that you wish to ask and indeed answer.
For instance, any attitudes to hearing aids should be assessed before the test, because any conversations that you have around BTEs versus ITEs, binaural versus Monaural, lifestyle needs, medical contraindications to certain devices etc will be seen as advice at this stage. After the test it will be perceived as you selling your point of view. Every professional should use the COSI and integrate it into their consultation, I have written of it before and I still think it is one of the most powerful tools which encourages emotional connection with your Patient and allows you to really understand their lifestyle needs. It also allows you to clearly manage their expectations and to agree a roadmap for your Patients care. All of this from an A4 piece of paper that practically explains itself.
Client Orientated Scale of Improvement, COSI and its uses for your practice.
Emotional engagement is the key, when you make an emotional connection with your Patient it allows them to trust you and feel that you not only understand them, their needs and problems, but you care enough to try your damndest to fix those problems to the best of your ability. This is the key to Patient retention, the crux of the matter, if a Patient feels cared for, that they are not viewed as just a wallet with cash in they feel that they are in a worthwhile relationship. If they feel that they are in a worthwhile relationship, they will stay in it, not only will they stay, but they will tell others about the wonderful caring new friends they have found.
The point is simple, to keep a Patient and gain their friends, treat them like a human being, treat them like they matter to you, their problems matter to you and more importantly the outcomes of their care matter to you. Because these are the things that matter to them.